DIAGNOSIS & TREATMENT
Diagnosis: Vaginal Vault Prolapse
Treatment: Laparoscopic Sacrocolpopexy
Vaginal vault prolapse is very similar to uterine prolapse however the patient has had a hysterectomy and no longer has a uterus
Vaginal vault prolapse is prolapse (i.e. lack of support) of the deepest 30% of the vagina. This area of support is the most crucial area for the overall support of the vagina. Vaginal vault prolapse is very similar to uterine prolapse however the uterus is no longer present as the patient has had a hysterectomy. Rarely does vaginal vault prolapse occur without other forms of prolapse such as a cystocele, urethrocele, enterocele or rectocele usually accompany it. Patients often suffer from a bulge in the vagina, pressure, vaginal pain, and lower back pain.
Normal Vault Support
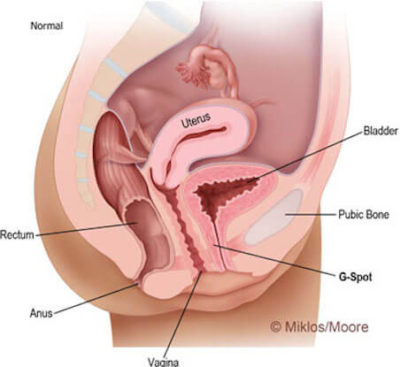
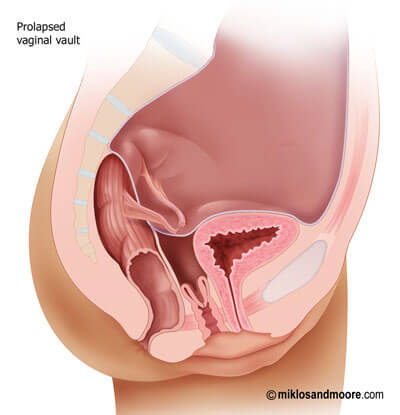
Vaginal Vault Prolapse
Laparoscopic sacrocolpopexy is the “gold standard” operation for support of the vaginal vault for almost 50 years. It is the most successful operation ever developed for vaginal vault prolapse and is considered the gold standard by the American Urogynecologic Society and the US FDA. Dr. Miklos & Dr. Moore have performed more than 1600 laparoscopic sacrocolpopexies, more than anyone in the world with minimal complications. Surgeons from throughout the world travel to Drs. Miklos and Moore’s Centers on a regular basis to learn this advanced procedure.
Does Insurance Cover Vaginal Vault Prolapse Surgery?
If you have UMR insurance, your plan may provide coverage for vaginal vault prolapse surgery when the procedure is deemed medically necessary. Vaginal vault prolapse is a functional pelvic floor disorder that commonly causes pelvic pressure, vaginal bulging, urinary dysfunction, and discomfort following hysterectomy. Because vault suspension surgery is performed to restore pelvic support and correct these symptoms — not for cosmetic purposes — many UMR plans include benefits for prolapse repair.
As leading Atlanta prolapse surgeons, our office routinely works with UMR insurance to verify benefits, obtain any required authorizations, and help patients understand their financial responsibility before surgery. We are committed to ensuring that women seeking advanced pelvic floor reconstruction have access to both expert care and clear insurance guidance.
Vault Prolapse

Laparoscopic Sacrocolpopexy
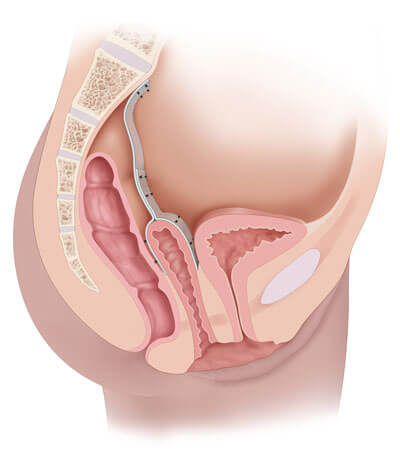
Dr. Miklos & Dr. Moore Experience
Laparoscopic Sacrocolpopexy
Experience
> 1600 cases
98% cure rate
50 minutes
Minimal pain
1-day hospital stay
Laparosocpic Sacrocolpopexy
Complication Rate
< 1/1000 blood transfusion
1/500 mesh infection rate
< 1% bowel injury rate
< 1% bladder injury rate
< 1% ureter injury rate
