Sacrocolpopexy Mesh Complications
The sacrocolpopexy is a mesh implant which is considered the gold standard procedure to treat vaginal vault prolapse which can result in a mesh complication such as mesh erosion or vaginal pain.. . It has the highest cure rate in the literature and has been studied for many years. It is a procedure where a Y-shaped piece of mesh is placed over the top of the vagina and down upper anterior and posterior walls of the vagina and then the other end is attached to a ligament on the sacrum. This holds up the top of the vagina, the top of the bladder and rectum. Complication rates are relatively low; however, mesh complications still occur. The rates of mesh complications compared to vaginal placement of mesh seems to be lower, however it is a much more invasive operation (especially when done via laparotomy or a large open abdominal incision). Drs. Miklos and Moore recently published the largest series in the world on Laparoscopic Mesh Sacrocolpopexies and had an overall complication rate of less than 1% (click here to see paper). However as with ANY prolapse surgery, with or without the use of mesh, complications the CAN still occur.
Types of Complications
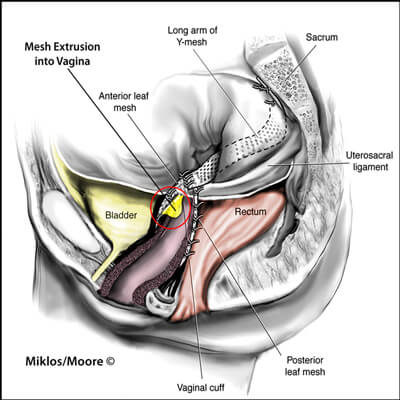
VAGINAL MESH EXTRUSION/VISIBLE MESH
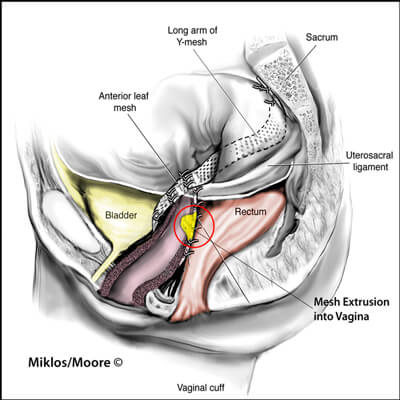
VAGINAL PAIN/PAINFUL INTERCOURSE
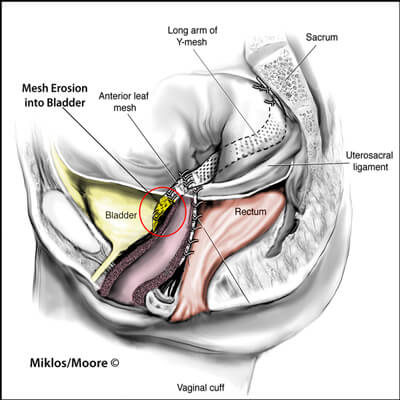
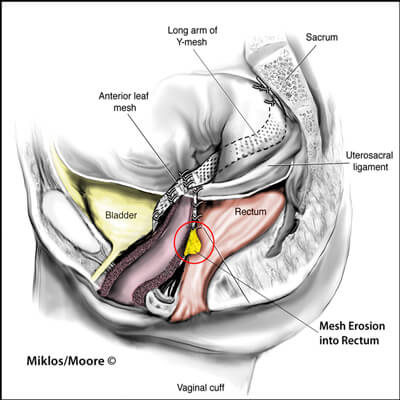
MESH EROSION BLADDER/RECTUM
INFECTION/ABSCESS OF MESH





Drs. Miklos and Moore are world experts and innovators in laparoscopic treatment of mesh complications. They are researchers who are widely published in the world’s leading journals.
However, all surgeries can have complications even those utilizing an abdominal approach to place synthetic mesh. Drs. Miklos & Moore have more experience than 99% of surgeons in the world removing sacrocolpopexy mesh and they are two of few surgeons in the world who can remove the mesh through miniature incisions ie laparoscopically.
TREATMENT
Not all patients with mesh erosions are symptomatic. Some patients have no symptoms whatsoever. It has been Drs. Miklos & Moore’s’ experiences that mesh erosions through the vaginal skin without symptoms need not be treated, as it is not dangerous to the patient. However, patients suffering from the symptoms of mesh extrusion have a choice between non-surgical and surgical treatment.
In small cases of mesh extrusion the first line of therapy is treating with transvaginal estrogen cream. Applying estrogen every day x 14 days and then 2-3 times per week there after can sometimes help the vaginal skin heal over the mesh extrusion.
In patients with large areas of mesh extrusion or in patients who have failed transvaginal estrogen therapy the next option is surgical removal. Patients can usually have their mesh removed through the vaginal opening with a single incision in the area of mesh exposure. In more advanced cases the complete mesh needs to be removed and this often requires an abdominal approach and in Drs. Miklos & Moore’s hands they perform this using a laparoscope.
