DEFINITION
Lichen Sclerosus (LS) aka Lichen Sclerosus et Atrophicus is a dermatological genital disease that can be life-changing for many women. It is a chronic inflammatory dermatosis which is progressive and primarily involves the vulvus and anus. LS can be found in men, women or children however postmenopausal women are more commonly affected. While the exact cause of Lichen Sclerosus is unknown, several correlating factors have been identified. Autoimmune diseases, genetic risk factors, inflammatory responses, infections and hormonal imbalances are commonly associated as potential causes. One study suggests genetics may play a role in some patients. A Review of over 1000 patients with vulvar Lichen Sclerosus revealed a positive family history in 12%. As well, patients with previous injury or skin damage to a particular area seems to increase the likelihood of Lichen Sclerosus at that location.
86% of Patients Achieve Resolution of Lichen Sclerosus Symptoms Through Treatments with FormaV and Morpheus8V
This breakthrough prospective study explores the effects of bipolar radiofrequency (RF) with microneedling to treat the vaginal and vulvar symptoms of Lichen Sclerosus (LS), a chronic inflammatory condition affecting the genital skin and mucosa in women. Traditional treatments, especially corticosteroids, often fail to provide long-term relief. Patients in this study underwent a series of combination treatments using EmpowerRF’s FormaV (bipolar RF) and Morpheus8V (RF with microneedling). The results showed a significant improvement in LS symptoms. >> Read more
PHYSICAL FINDINGS
Upon physical examination, atrophic dermatologic changes are noted. White, silvery plaques may be noted to the labia minora, labia majora, perineum and anus. Epithelial thinning is present, causing fragility of skin. With progression of the disease, the labia minora and majora lose distinction. This indiscretion causes the clitoris to become concealed and the introitus to close. Fissuring and excoriation of the skin may be present due to severe scratching.
In men and women, LS is usually a scarring, progressive and relapsing lifelong condition. Overtime Lichen Sclerosus can cause obvious and prominent changes to a woman’s vulvar anatomy including: resorption and fusion of the labia minora, entrapment of the clitoris (phimosis) and the vaginal opening (introitus) can become narrowed and stenotic.
BEFORE AND AFTER PHOTOS OF LICHEN SCLEROSUS TREATMENT
Individual results may vary
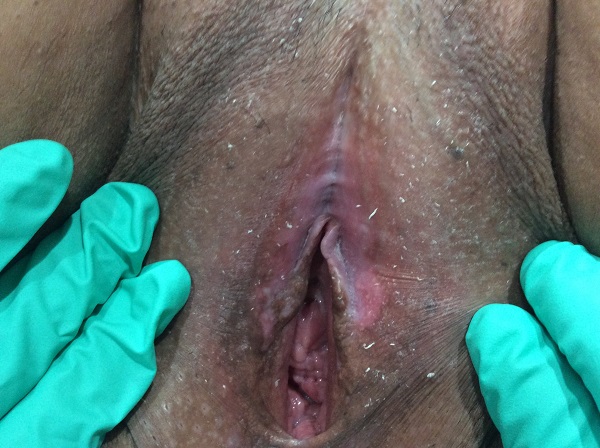
Before
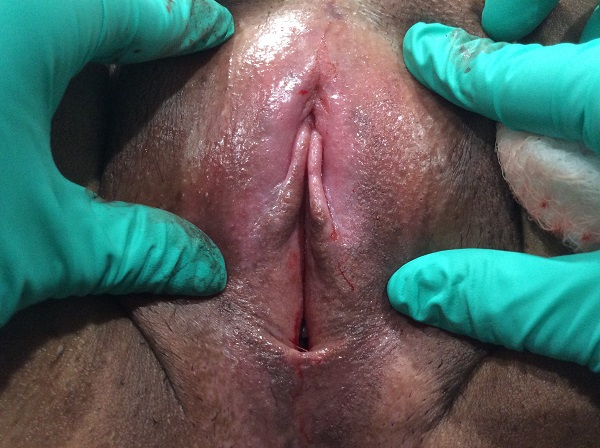
After
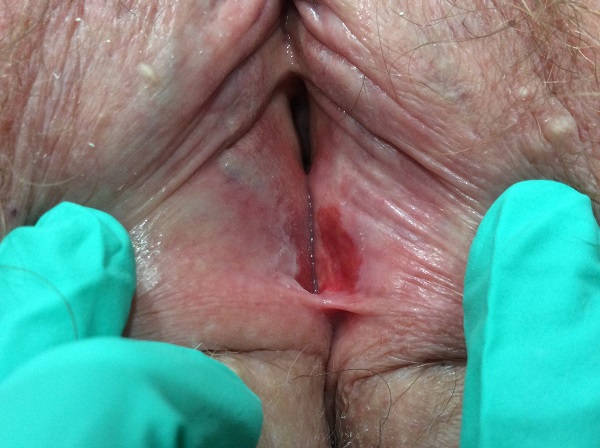
Before
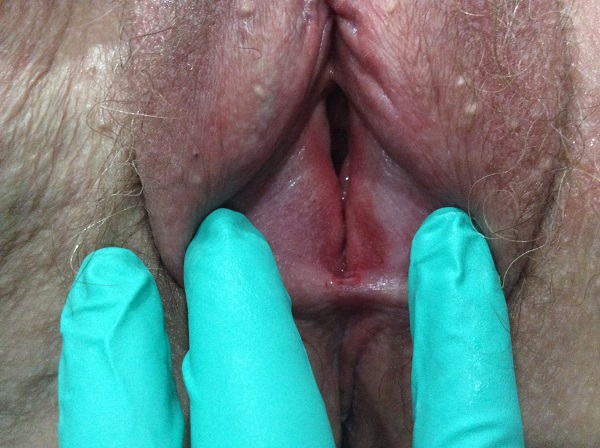
After
Patient: “Just a follow-up on my previous comments, the Morpheus treatments have changed my life. It has been 11 years since I have been able to have intercourse without me crying from pain. After 2 Morpheus treatments, intercourse is so much less painful. The lichen sclerosis is no longer an issue and we are on our way to a normal physical relationship once again. The doctors and staff have been wonderful here and will be referring any friends that need “rejuvenated” to this office.”
–Very thankful
SYMPTOMS
Women with LS may be asymptomatic or exhibit one or more symptoms. Pruritis (itching) and irritation is the most common symptom associated with Lichen Slerosus. Vulvar pain and discomfort to the perianal area has also been documented. Dysparenuia (pain during intercourse) is common among women with Lichen Sclerosus due to inflammation, fragility of skin, introital closure and excoriation. Other signs and symptoms may include:
- Smooth white skin spots (vulvar and perianal)
- Skin bruising
- Skin tears
- Bleeding, blistering, ulcerations
When the LS gets severe and encompasses both the vulva and the anal area the patient will often present with a Figure of “8” pattern. Where the atrophic skin around the vulva and anus as well as across the perineum is white, thin and atrophic.
The severity of symptoms varies from patient to patient. While some women are not affected or are asymptomatic, other women’s symptoms can interfere with a patient’s quality of life and specifically their ability to enjoy intimacy.
DIAGNOSIS
Diagnosing Lichen Sclerosus is generally completed through physical examination, presenting symptoms and biopsy of vulvar tissue. A biopsy is used to confirm diagnosis and rule out differential diagnoses. Several other disorders may mimic LS and be difficult to differentiate without a confirmatory biopsy. Differential diagnoses may include lichen planus, vulvar dermatitis, atrophic vaginitis, mucous membrane pemphigoid, candidiasis, psoriasis, cancer and hormonal deficiencies.
TREATMENT
Treatment options vary and are discussed on an individualized basis with each patient. Women may decide to forgo treatment if they are asymptomatic or their quality of life is not affected. Traditional treatments which have been used for decades include:
Topical corticosteroids are considered the first line therapy in the treatment of LS. The corticosteroids are applied for 6-12 weeks as the initial course before moved to maintenance therapy. Others have suggested using emollient creams for maintenance therapy. Corticosteroids include: clobetasol propionate (Clobex, Temovate, Olux) , Diflorasone diacetate, fuoinonice ( Vanos) . A large study of 74 girls with LS were treated with topical corticosteroids; 72% became symptom free, 25% experienced subjective improvement, 22% showed complete resolution and 67% showed partial resolution of clinical signs. However, usually a need for maintenance therapy is required due to the high rate of recurrence. If corticosteroid therapy fails, additional therapies may be initiated.
Topical Calcineurin Inhibitors (TCI), pimeocrolimus and tacrolius have anti-inflammatory activity and immunomodulatory effects. There have been several reports which advocate the use of TCI in the treatment of LS and have stated they are safe and effective. Yet other researchers and scientists have objected to its use for fear of increasing the chance of some sort of malignancy. In the U.S., the use of TCI in patients with LS is off label.
Pimecrolimus was first reported in 2004 for use in children. A 1% twice daily application resulted in “considerable improvement” of signs and symptoms within 6 weeks of treatment and almost complete remission with in 12-16 weeks of treatment.
Tacrolimus was first reported for use in patients with LS in 2003 and 2005. A total of 8 patients achieved complete remission after 6 weeks to 10 months of treatment. After 3 months of treatment 12.5 % had achieved complete resolution. In a large study of 84 patients with LS, patients were treated with tacrolimus 0.1% twice per day for 16-24 weeks. Complete remission was achieved in 43% and partial remission in 34 % of patients.
Topical Retinoids have been shown to be useful in the treatment of LS but have not become widely accepted in the treatment of vulvar LS. This probably due to their well-known adverse effects and the need of long-term treatment.
Surgery is also an option but commonly used as a last resort. It has often been suggested that surgery for LS should be limited to patients who have a precancerous condition known as vulvar intraepithelial neoplasia (VIN), cancer, or to correct scarring interfering with normal function. Vaginal opening (introital) narrowing may lead to difficult with urination or sexual intercourse and may require widening. Surgery should not be performed until the disease activity has ceased.
Photo and Photodynamic Therapy (PDT) is a reasonable option in cases of conventional treatment resistance. One of the most recent studies of 100 women with genital LS treated with PDT revealed a partial or even full remission of subjective symptoms and objective clinical signs could be observed.
Radiofrequency- RF (ThermiVa) –Here at Miklos & Moore Urogynecology we have had good success using a new treatment modality known as radio frequency. Using the painless modality of RF along with injections of either hyaluronic acid or platelets, we are seeing a dramatic improvement in clinical signs and symptoms and especially in vaginal pain with intercourse and vaginal introitus narrowing. Usually a patient needs to complete 3-4 treatments within 6 months followed by additional treatments annually after remission. Please note: The ThermiVa system and probes are FDA cleared (K130689) and indicated for use in dermatological and general surgical procedures for electrocoagulation and hemostasis; creation of lesions in nervous tissue.
CONCLUSIONS
Despite evidence of autoimmune etiology in genetically predisposed patients, the cause of Lichen Sclerosus remains unknown. Infectious causes such as B. Brudorferi is still unproven and hormonal influence seem unlikely. Lichen Sclerosus may lead to scarring, distortion and disruption of the vulvar architecture and in a large proportion of affected individuals may cause sexual dysfunction. The diagnosis of LS is usually clinical but in clinically unclear cases a histological examination is required. Topical corticosteroids are highly effective, and remain the first – line of therapy and they often give symptom relief in the first few days. Emollients are recommended as supportive therapy. TCI is utilized in cases which are unresponsive to corticosteroids and may require 24 weeks to obtain an optimal response. Surgery should be limited to those conditions associated with malignancy or for patients who have severe scarring restricting micturition or sexual function. New modalities such as radiofrequency and Hyaluronic acid or platelets have shown to be both safe and effective in patients who are not responding to topical agents.
Cooper, S.M., & Arnold, S.J. (2017). Vulvar lichen sclerosus.


